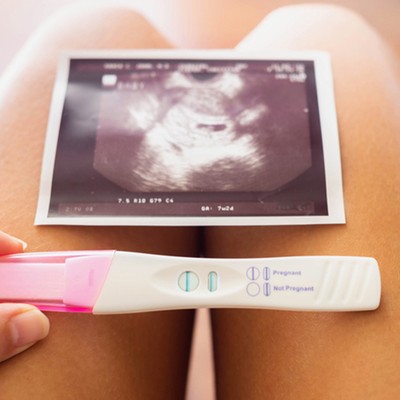
Our IVF Journey: Lucy & Amy
Lucy: We’ve been together for nine years and originally met in London, although neither of us lived there at the time. Back then, neither of us were out, but if anything, the fact no one knew made the relationship a bit more fun.
Amy: I knew my family would ask a lot of questions and I didn’t feel the need to get into all that. Our relationship was also long distance for over a year before we both moved to London – Lucy for work, me for university.
Lucy: Our relationship had turned serious by this point, and I ended up proposing about five years ago in Palm Springs – it was then that Amy felt she should reveal our relationship to her family.
Amy: After Lucy's proposal, the first thing I felt was pure panic at the thought of having to have the conversation. That night, I decided to send my family a text message – everyone was so supportive and kind; they were really happy for us. To this day, though, we’re still only engaged. We decided pretty much there and then to put our money towards becoming parents instead.
Lucy: We’d always discussed having a family and about a year after getting engaged – around 2017 – we set about getting more information from our GP. We couldn’t find anything that helpful online about gay couples trying to have a child together, but the GP said he would make some calls and get back to us. A letter eventually came through the post saying we’d been referred to a fertility clinic, which came as a bit of surprise. Although we both wanted a baby, I’ve always had more of a desire than Amy to be pregnant, so it was an easy decision as to who out of the two of us would carry the baby.
Amy: We’d worked out we probably wouldn’t be eligible for any NHS treatment. In fact, we realised we had to self-fund six rounds of intrauterine insemination (IUI) – a fertility treatment that involves directly inserting sperm into a woman's womb with a catheter in a medical setting – in order to qualify for one round of IVF on the NHS. Even then, the requirement was that all the IUIs needed to come back negative for us to receive free fertility treatment. We started medicated IUI at the beginning of 2018.
Lucy: Medicated IUI meant we were monitored by a clinic, where they also stimulate your follicles and give you a trigger shot to make you ovulate. It helps them time the IUI more precisely. The difference with natural IUI is they follow your natural cycle, you then take ovulation tests and when you’re ovulating, you let the clinic know and they book you in for the IUI. The medicated version felt right because it gave us more control. It was the more expensive option, though. One round of IUI is roughly £700, with one vial of donor sperm coming in at around £800. The storage of that sperm can top roughly £300, and all the admin and medication came to more than £400.
Amy: Finding the sperm was one of the most enjoyable parts for us. We took it seriously, but we had fun with it too. Some people really struggle with it. We picked some sperm banks based on recommendations from our clinic. Each of us looked separately and then we sent each other candidates we liked and compared to see if there were any that matched up. It helped us narrow the search. We could see an adult picture and baby picture of the donors and read up on their different personalities and family medical histories etc.
Lucy: When the first three IUI cycles came back negative (i.e. I didn’t fall pregnant), we felt our hearts couldn’t take much more. The success rates aren’t great – the chances of falling pregnant with IUI is about the same as a heterosexual couple having sex just one time. Anyway, our disappointment combined with a better understanding of the slim chance of success made us look for a private fertility clinic. We decided to up our chances of success and self-fund the rest of our treatment. We worked lots of extra shifts, saved like crazy and then handed the money over.
Amy: We did three cycles of IVF – essentially egg retrievals – at the new clinic and during the first cycle, Lucy donated half of her 11 eggs, which helped bring the cost down. We knew how grateful we were to our sperm donor, so it was wonderful to think we might be able to help someone else start a family. We kept six and gave away five. We transferred one embryo of our own and didn't have any embryos leftover to freeze. Sadly, Lucy bled through the two-week wait, which resulted in what they call a 'chemical pregnancy' (a very early miscarriage). The couple we donated to also didn't get pregnant or have any more embryos to freeze. Suffice to say we booked a holiday after all of this – we needed a bit of an escape!
Lucy: I never found the egg retrieval that unpleasant. They sedate you and I was just a little sore afterwards. The more rounds we did, though, the bigger the effect on my body, especially in terms of the fatigue and feeling very swollen. But that probably had less to do with the treatment itself and came down to stamina. It’s exhausting.
Amy: The second round of IVF ended up being a fairly similar experience. We slightly changed how Lucy was taking progesterone – this time with injections which are suspended in oil – which made the whole thing a bit more intense. They’re large needles and if you don’t warm up the oil properly, it can collect under the skin. In total, I think Lucy had about 290 injections over the three years of fertility treatment. Sadly, this IVF attempt resulted in another chemical pregnancy.
Lucy: The third time, we managed to get to six weeks, but I ended up miscarrying at the seven-week scan just before Christmas 2019. Thankfully, this time we had four viable embryos leftover – during rounds one and two this hadn’t been the case. It meant we had ‘spares’ in the freezer so to speak, so we could do a frozen embryo transfer in the future without having to do another egg retrieval.

Amy: When we fell pregnant again in the middle of 2020, it still wasn’t an easy experience. We’d had two embryo transfers cancelled as a result of the pandemic and even though the July transfer was successful, Lucy ended up bleeding through the whole of the first trimester. We both had lots of anxiety following the 2019 miscarriage, too. I’m a nurse and had been working a night shift when Lucy called me to say she’d woken up bleeding. I came home but we both went back to the hospital to the early pregnancy unit, but they wouldn’t let me into the room with her. It was the same room where they’d told us Lucy had miscarried at Christmas, and I completely lost it.
Lucy: Thankfully, a woman there recognised me and let Amy in because they knew us. Better still, the doctor told us the baby was fine – I was just one of the unlucky few who experience quite a bit of bleeding at the start of a pregnancy. It’s quite common with frozen embryo transfers apparently – especially when you’re taking lots of oestrogen.
Amy: There are so many things they don’t tell you because they don’t want you to worry, and that’s good. But then, when something does happen, you wonder why no one’s prepared you for it. I like knowing as much as possible beforehand, but I’m sure that’s not the case for everyone.
Lucy: After waiting three years to be pregnant, we opted to go to a Harley Street clinic to do what’s called the Harmony Test – a blood test that checks for chromosomal problems, as well as the sex of the baby. We found out at 12 weeks we were having a boy. We’d really wanted a boy, but after all this time, we only cared about having a healthy baby. That said, it made everything feel like it was ‘meant to be’.
Amy: I came up with the name Nathanial years ago – I’ve always loved it.
Lucy: I said no when she first told me!
Amy: She vetoed it initially, but when Lucy was pregnant, she suddenly turned to me one day and said, “What about Nathanial?” I couldn’t believe it. I said, “That was my suggestion!” Anyway, it stuck. We didn’t want to commit to anything until he was born, but we kept referring to him as Nathanial throughout the pregnancy.
Lucy: From about the ten-week point – once we’d decided to do the Harmony Test – I noticed my heart rate going up and started feeling increasingly out of breath. I just knew it wasn’t right. I was diagnosed with Postural tachycardia syndrome (PoTS) – an abnormal increase in heart rate that occurs after sitting up or standing.

Amy: It got to the point where she was so exhausted she couldn’t do much more than lie on the sofa – but thankfully we were mainly at home because of the pandemic. There’s not a lot you can do for PoTS generally, and even less so in pregnancy. The doctors told us to carry on as best we could but nothing we did – adding more salt to her diet, upping her hydration – made much difference. I was scared something would happen to Lucy at this point – especially when they recommended she have a vaginal delivery. She was the most important person in my life and I didn’t know how she could cope with a natural delivery when she was so fatigued already.
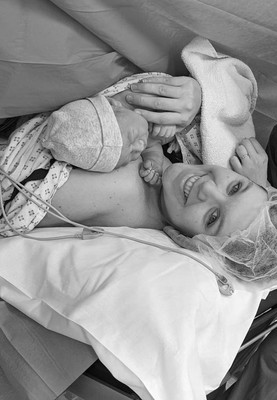
Lucy: I didn’t know how I would manage to push a baby out either – especially with Amy not allowed on the post-natal ward. Suffice to say we opted for a C-section, and our consultant was so supportive of that decision – she agreed it was for the best if it made me feel more comfortable. In the end, when I gave birth on April Fool’s Day, having a caesarean was such a positive experience. He was 3.8kg of total perfection.
Amy: After the birth, I was so emotionally drained – largely because of the pandemic and everything we’d coped with up until this point. I’d also seen lots of new mums ventilated in intensive care as a result of Covid. By the time Nathanial was born, things had eased up a bit and I was allowed into the C-section, the recovery room and had a two-hour time slot on the postnatal ward. All things considered, we were grateful to have that time together.
Lucy: By the second day I was cleared to go home, but those first few days with a newborn are a massive blur. We were so happy and grateful to have him home, but we were so tired.
Amy: I was also very anxious – in fact, we took three trips to A&E because I was convinced there was something wrong with the two of them. Nathanial was a bit jaundiced but didn’t need treatment and I was convinced Lucy’s C-section scar was infected – it wasn’t!
Lucy: I think breastfeeding was the hardest challenge of for me. In recovery, I managed to get a good latch and my milk came in nicely, but when it came to cluster feeding, no one tells you that the extreme exhaustion and cracked, bleeding nipples are completely normal. You can’t do anything but sit there and feed. Amy was very involved, though – I would lie on the sofa with him attached to my boob and fall asleep while she kept watch to make sure I didn’t suffocate him!
Amy: Nathaniel is incredible – we’re so in love and can’t believe he’s ours. He’s made everything we’ve been through feel worth it. It blows our mind to think if the other IUI or IVF rounds had been successful, we wouldn't have him – it would be a completely different baby. Lucy hasn't had any problems with her heart since giving birth either, but she will have cardiology follow ups in the future.
Lucy: We definitely want more children – we plan to use the frozen embryos and hope that they work. If not, we’re not sure what route we’ll take. Unfortunately, the sperm donor we used has now retired and we don’t have any of his sperm left in storage. Nathaniel came from the last vial of donor sperm we had in the freezer. I’ll give Amy first refusal on the pregnancy this time – I’d be completely happy if she said she wanted to experience it first-hand.
Amy: If I could say anything to other couples, it would be focus less on the money and prioritise looking after yourself emotionally and physically. IVF consumed us – even though we tried hard not to let it – and I wish we’d had a bit more fun along the way. Even with the miscarriage, we should have hung onto the happiness we felt in the run up to the seven-week scan, rather than the grief that followed. But we’ve always worked well as a team, and as two new mothers, it’s exactly the same. We just feel so grateful to be able to look after our beautiful baby boy.
You can follow more Lucy & Amy’s pregnancy journey @OurBigGayJourney on Instagram.
DISCLAIMER: Features published by SheerLuxe are not intended to treat, diagnose, cure or prevent any medical issue. Always seek the advice of your GP or another qualified healthcare provider for any questions you have regarding a medical condition, and before undertaking any diet, exercise or other health-related programme.
DISCLAIMER: We endeavour to always credit the correct original source of every image we use. If you think a credit may be incorrect, please contact us at info@sheerluxe.com.


